A New Set of Healthcare Priorities for Policymakers
Just a few days after the dramatic collapse of efforts to pass the House GOP’s American Health Care Act, more than 1,300 folks with an interest in employer-sponsored health benefits joined a Mercer webcast* to learn a) what the heck just happened, b) now what, and c) what does this mean for employer health benefits? A team from our Washington Resource Group aced the first question and gave as good a look into the future as possible without a crystal ball.
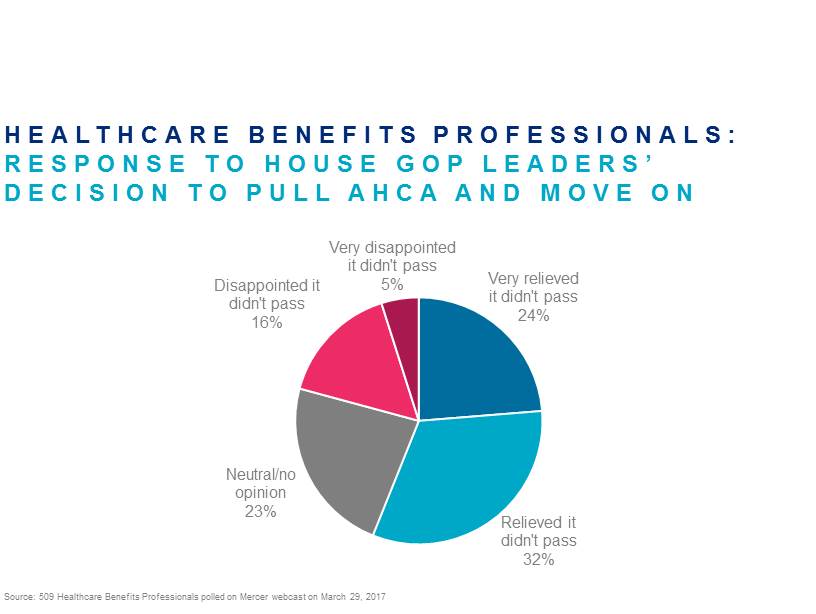
We took advantage of the opportunity to ask the health benefit professionals on the call a couple of questions, starting with their reaction to the (apparent) death of the bill. More respondents were relieved than disappointed; in fact it wasn’t even close. Enough said.
Our second question was inspired by our belief that while shoring up the individual market and ensuring Americans have access to affordable health coverage is critical, neither the AHCA nor the ACA did nearly enough to address the underlying problem in the US healthcare system: too much cost for not enough value. Given that employers provide coverage to more than half of all Americans, employers are key stakeholders in any effort to reform US healthcare. So what would they like Congress and the administration to prioritize going forward?
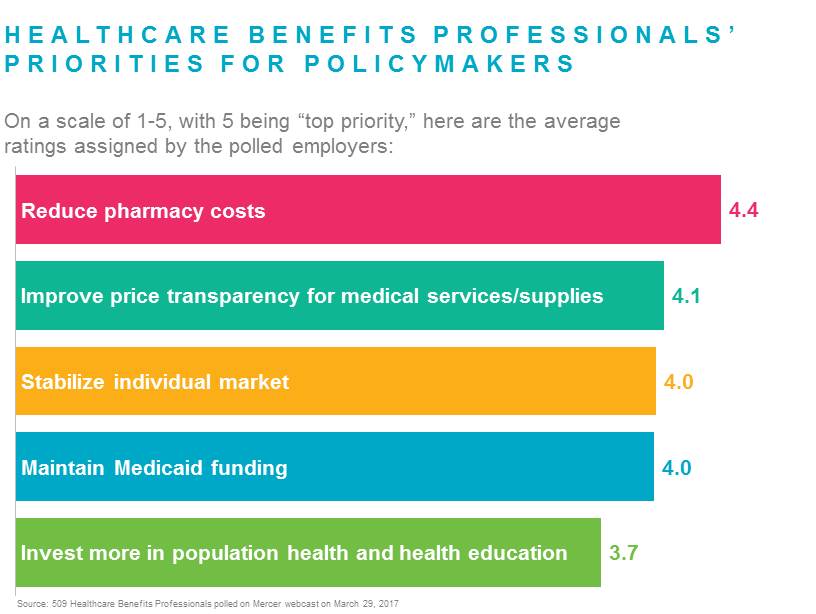
At the top of the wish list is help with controlling the escalating cost of pharmaceuticals: on a scale of 1-5, that scored a 4.4. Next was improving price transparency for all medical services and supplies. Most respondents to the poll also want the government to maintain Medicaid funding and stabilize the individual market so that people not in employer-sponsored plans have access to affordable coverage. A rise in the number of uninsured will increase providers’ risk for uncompensated care, leading them to hike rates for private payers. This type of cost shifting does nothing to address the underlying cost of care and makes it harder for employers to provide affordable coverage.
As we’ve been saying, employers are uniquely positioned to help control healthcare spending and promote positive health outcomes. They are working to help employees become responsible insurance consumers and are a trusted source of health information and resources. Policymakers should view this health reform “reboot” as an opportunity to partner with American businesses to drive higher quality, lower costs, and better outcomes for all Americans.
*Mercer Select Intelligence membership required. Not a member? Learn more
