Health Plan Coverage Benefits Parity At Workforce
It’s well known that working women earn less money than their male counterparts, but they may also be at a disadvantage when it comes to health benefits. Using data from Mercer’s National Survey of Employer-Sponsored Health Plans, we compared companies with workforces that are 65% female or more to those with workforces that are 65% male or more. About half of the mostly female companies are in health care and about a quarter are in the services sector, while mostly male companies are found predominately in manufacturing. The percentage of employees in collective bargaining agreements is about the same for the two groups, at just under 15%. Not surprisingly, when the workforce is mostly female, the average salary is about $10,000 less than when the workforce is mostly male.
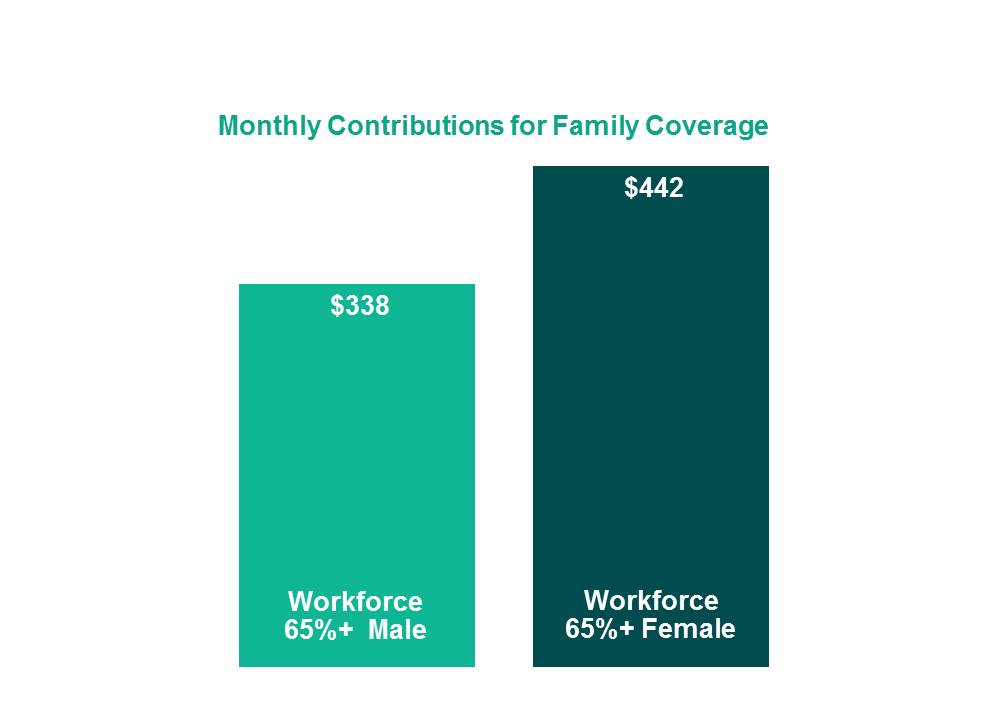
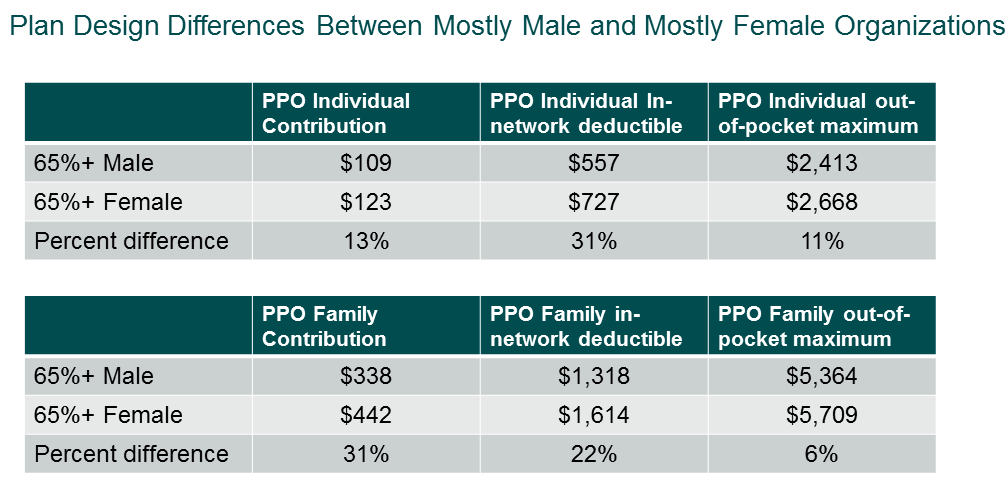
Pay and benefits tend to go hand in hand. The health benefits at organizations with predominantly female workforces are also less generous than in those with predominantly male workforces. Because women generally use health services more than men, the disparity in benefit levels has an even greater financial impact. Women use maternity services, and childbirth, the leading cause of hospitalization in the US, accounts for a quarter of all hospital stays. We found that average employee contributions as a monthly dollar amount are higher in mostly female companies: For coverage in a PPO, the most common type of medical plan, the monthly contribution for family coverage is 31% higher. In addition, average in-network and out-of-network deductibles and out-of-pocket maximums are consistently higher. For example, the average in-network PPO deductibles in mostly female companies are $727 and $1,614, respectively, for individual and family coverage, compared to $557 and $1,318 at mostly male companies.
And the benefit gap doesn’t end with active employment. Mostly male companies are also more likely to offer retiree medical benefits — 27% offer medical coverage to pre-Medicare-eligible retirees, compared to just 19% of the mostly female companies.
The Affordable Care Act (ACA) targeted some health plan coverage practices that discriminated against women. For example, health plans are now required to cover “essential benefits,” which include maternity and newborn care, an annual mammogram for women starting at age 40, and domestic violence screenings. Due to the ACA, most women enrolled in employer-sponsored plans now have access to free contraception. In addition, in 2015, when the Employer Shared Responsibility mandate goes into effect, more US employees will have access to employer-sponsored coverage as companies are required to extend coverage to all employees working 30 or more hours. The industries most affected by this new rule are those with large populations of part-time workers — which also tend to be industries that employ a lot of women. Currently, about a third (36%) of companies with mostly female workforces do not provide coverage to all employees working an average of 30 or more hours per week. They will be required to do so in 2015.
It is important for all employers, and especially those with largely female workforces, to understand the difference in how men and women use health benefits to ensure that plans meet their needs in an affordable manner. One solution may be to offer a range of choices that allow workers to choose between plans with lower premium contributions and higher deductibles, and plans with higher up-front cost but lower cost sharing. Thoughtful dependent coverage tiers and salary-based contributions can also address equity concerns. Because women use health benefits more, it stands to reason they value them more. For employers with a mostly female workforce, the right health benefit package might be the key to a more engaged, productive, and loyal workforce.
Alyssa Grabfield from Mercer conceived and performed the data analysis and assisted with the reporting.
