Contact Tracing at Work, Works -- and it’s Not That Complicated

While the US continues to grapple with controlling the COVID-19 pandemic, Mercer continues to work with employers in mitigating the impact of the coronavirus on employees and businesses. The last four months have been a time of rapid learning, exponential discovery and creative adjustment. We now know we can limit the spread by keeping physical distance, wearing cloth facemasks, washing hands, cleaning and disinfecting, and improving building airflow. But another strategy hasn’t received the attention it deserves: Contact tracing, which has been used for centuries to slow the spread of infectious disease. While contact tracing is the responsibility of public health officials in the U.S., they have been stretched too thin to manage the demand in many areas. Employers seeking ways to improve worksite safety should consider a contact tracing program – because we know it works.
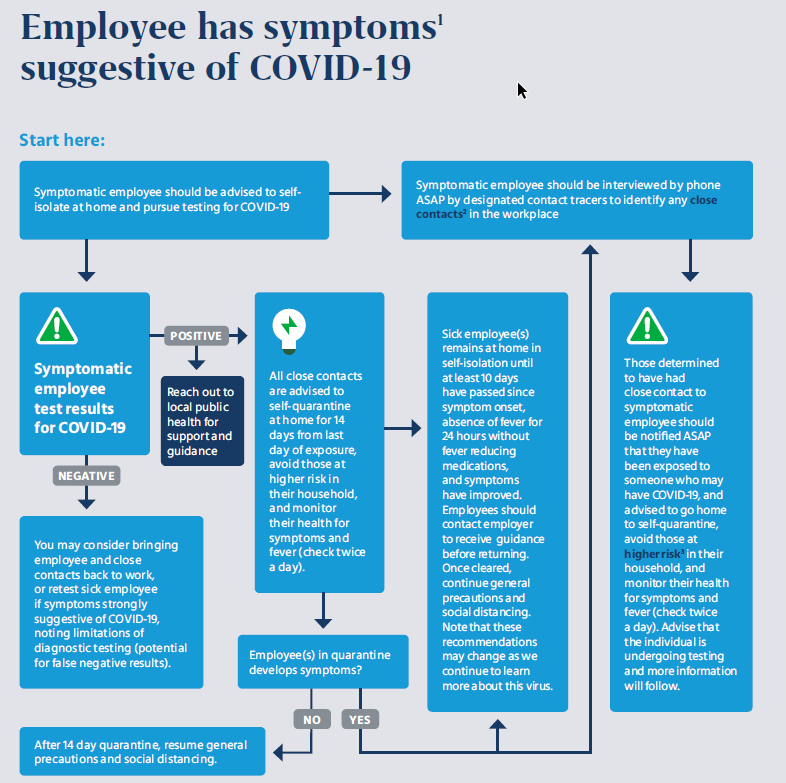
Unfortunately, a lack of direction and guidance around how to conduct contact tracing at the workplace is hampering employer efforts. A quick Google search turns up a lot of information directed at state and local public health officials, which applies only loosely to an employer, and a lot of ads for proximity tracking devices and apps. The good news is that contact tracing for employers doesn’t need to be too complex. Breaking it down into its parts can help, and creating a workflow to illustrate the steps, as we have done, can go a long way in creating clarity. Here are the key questions from an employer’s perspective:
- Who does it? Most often it’s an internal resource, typically within HR. Good communication skills are important and training and support is key.
- What triggers the process? Any symptoms suggestive of COVID-19. Don’t wait for a positive test result! Time is of the essence.
- What constitutes exposure? While CDC guidelines define exposure (i.e., close contact) as spending 15 minutes within six feet of an infected person, up to 48 hours before the onset of symptoms, depending on the work environment there are nuances that might warrant a more aggressive definition.
- What to tell contacts? Don’t disclose the identity of the infected individual. Close contacts should begin quarantine immediately, but testing will likely be most effective (i.e., the least likely to return a false negative results) 5-8 days after exposure. If a contact develops symptoms or tests positive, interview that individual to identify their close contacts.
- How long should a close contact quarantine? CDC recommends a 14-day quarantine even with a negative test. Some employers are following state or local guidance allowing quarantines to end earlier with a negative test taken 7 days or more after exposure.
- What type of testing? Consider pros and cons: RT-PCR performed in the lab is considered the gold standard in terms of accuracy (assuming tests are processed in a reputable lab). Point-of-care testing is faster but may be less accurate. In terms of the collection process, a self-swab is more comfortable and practical, and saliva tests, which are even more comfortable and practical, are becoming more common.
- Proximity apps? While controversial due to privacy and other concerns, they may be justified in factory and other settings where employees move around a lot. In office settings, an effective low-tech solution is for employees simply to record their contacts on a daily basis.
Employers would be wise to consult with legal counsel about any contact tracing strategy they choose, about applicable privacy laws, retention period for collected data, safeguarding the data, and potential anonymization techniques. Don’t forget to contact your local public health agency for support and guidance, and always review and understand local, state and national regulatory requirements.