Health Benefit Cost Will Rise 3.9% in 2020, Mercer Survey Fi

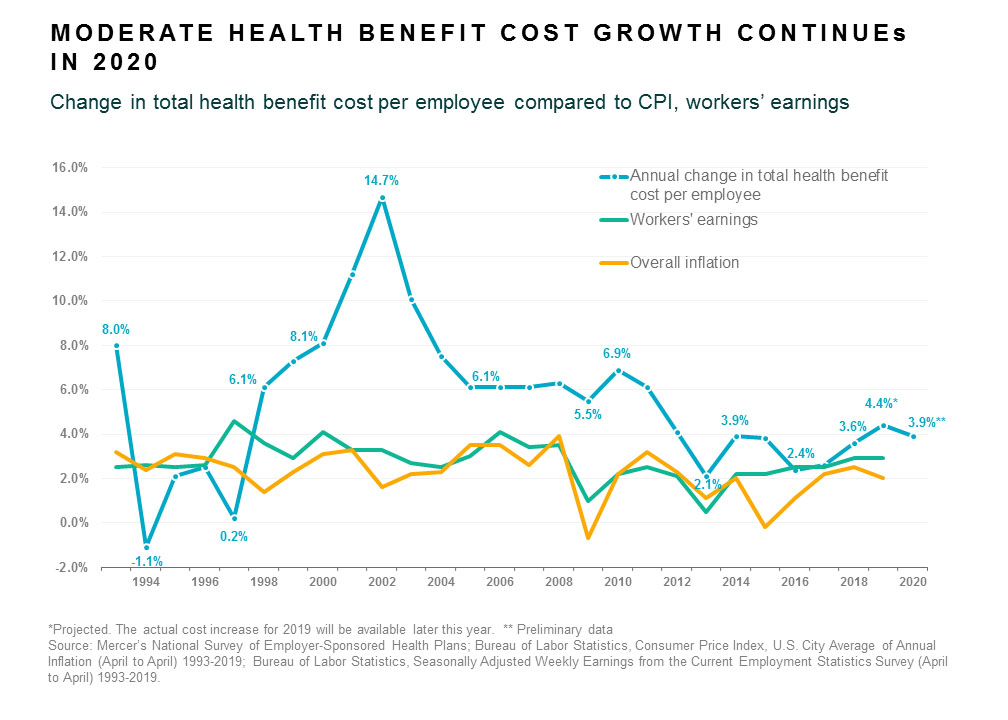
We’re excited to share some early results from our latest National Survey of Employer-Sponsored Health Plans – a sneak peek at the health benefit cost increase for next year. Based on the responses from the first 1,511 employers to complete the survey, we project that the average total health benefits cost per employee will rise by 3.9% in 2020. While this continues the trend of low single-digit increases that began in 2012, health benefit costs are still rising faster than overall inflation and employers know they can’t afford to be complacent – especially as economic growth begins to slow.
 Cost management efforts focus on improving health outcomes over cost-shifting
Cost management efforts focus on improving health outcomes over cost-shifting
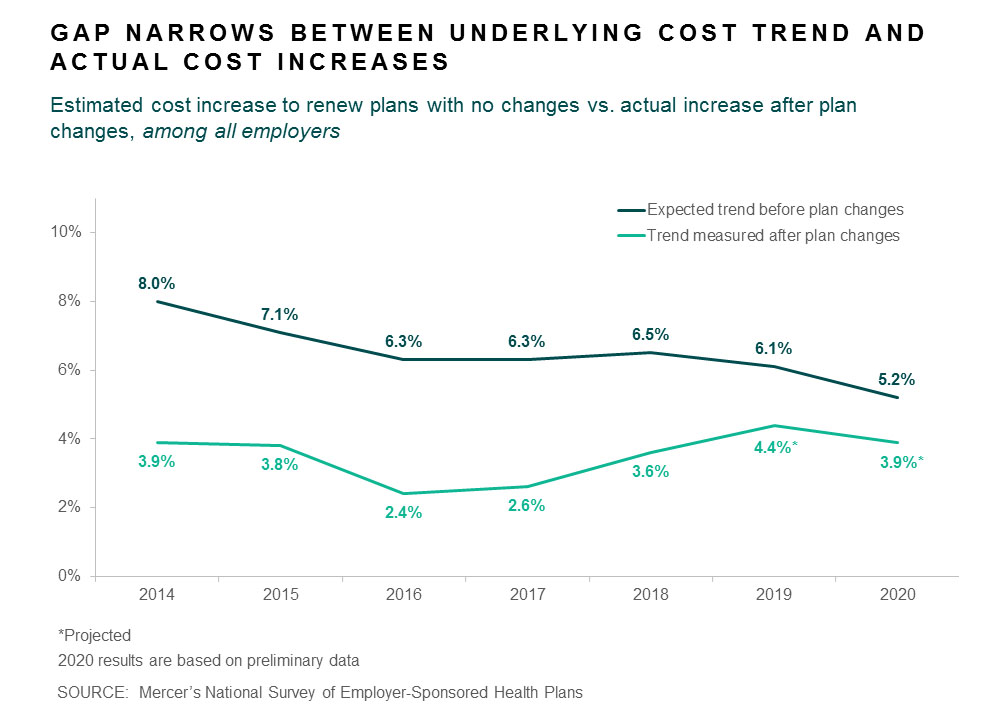
Early indicators are that cost-shifting to employees will be less of a factor than in past years, with just 43% of responding employers raising deductibles or otherwise cutting benefits to hold down cost in 2020. Since 2014, the underlying medical trend -- the amount that cost would rise if employers renewed plans without making changes -- has cooled from 8% to 5%, easing some of the pressure on employers to make short-term cost cuts.
Increasingly, employers have been adopting tactics that seek to reduce cost by improving health outcomes – for example, with targeted support for specific health conditions and by steering plan members to higher-quality providers. Rather than shift cost to employees, these approaches typically enhance the health care experience.
This year, employers continued to add tech-enabled programs designed to help members with health issues such as diabetes, insomnia, and infertility. Early results from our 2019 survey found that 62% of respondents with 500 or more employees now offer one or more of such targeted solutions, compared to 55% of employers this size in Mercer’s 2018 survey. A program for diabetes, for example, can significantly improve quality of life while reducing high-cost trips to the emergency room.
Improving access to health benefits information and resources is another growing trend. In 2019, 40% of respondents with 500 or more employees say that all or most of their benefit offerings are accessible to employees on a single, fully integrated digital platform – most often through a smartphone app – compared with 34% in Mercer’s 2018 survey.
Survey results also show employers taking action to help ensure plan members receive high-quality care. For example, 39% of employers with 500 or more employees now provide access to a Center of Excellence (COE) for cardiology, bariatric surgery, cancer and other complex treatments. Further, 16% say they steer employees to the COE by offering lower cost-sharing -- or even by requiring its use.
Employers have been experimenting with new approaches to tackle high costs, inconsistent quality, and low patient satisfaction. While there’s still so much more to do, it’s encouraging to think that we may be starting to see the positive effects of health innovation in the national health benefit cost trend.
The complete survey results based on responses from more than 2,500 employers with 10 or more employees will be released later this year, and will look at the full range of strategies employers are using to manage cost.
