HMO Use Shrinking Even as Interest in Integrated Care Grows
Both traditional PPOs and HMOs lost enrollment to high-deductible consumer-directed health plans in 2014, but for HMOs, the change resulted their dropping to third place among the three medical plan types. Just 16% of all covered employees were enrolled in an HMO in 2014, down from 18% the prior year. HMO enrollment peaked in 2000, at 33% of covered employees, but their slow decline seems to have been accelerated by the advent of CDHPs.
At the same time, there are signs that the integrated model of health care pioneered by the HMO is in favor again. More doctors’ offices are using nurses to handle general care and reserving physicians’ time for more complicated cases and annual physicals, as in the original HMO concept. Hospitals across the country are buying physician practices or partnering with doctors and health insurers to form accountable care organizations (ACOs) as a way of controlling more aspects of patient care. Doctors are also creating medical homes, where patient care is better coordinated. As in many HMOs, in these organizations, providers have financial incentives to provide quality, cost-effective care, including lump sums to provide comprehensive care for a specific condition.
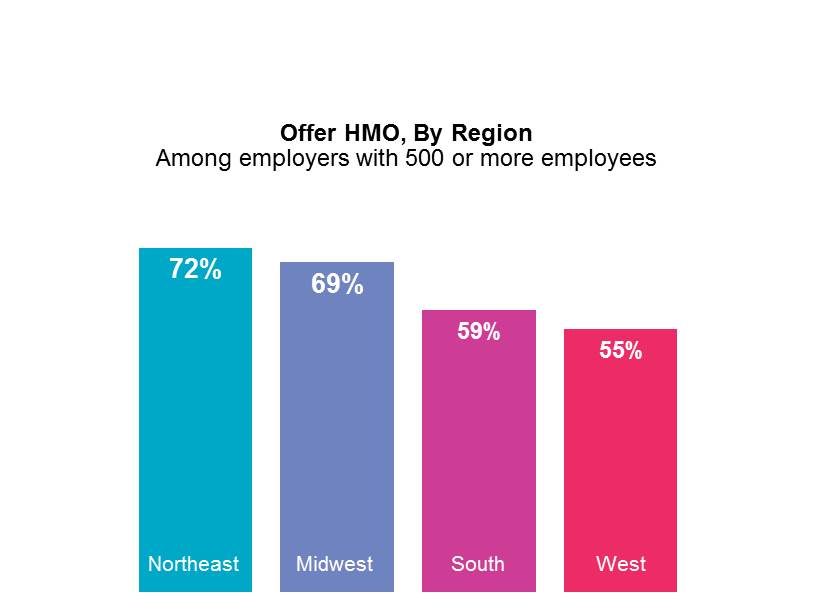
Nationally, HMOs are offered by 33% of large employers, but this ranges from 49% in the West to 27% in the Midwest. Per-employee cost averaged $11,719, compared to $11,121 for PPOs and $8,732 for HSA-eligible CDHPs. While employee cost-sharing remains generally lower in HMOs than in PPOs, over the past few years we have seen employers adding cost-sharing provisions as a way to stem rising cost. Where first-dollar coverage was one considered a hallmark of HMO coverage, today, a third of large HMO sponsors require an overall deductible (the median individual amount is $500), and 59% require a separate hospital deductible (the median amount is $250 per stay). In the original HMO concept, the use of primary care physician gatekeepers to authorize access to specialists was a key cost-control feature. However, more than half of large HMO sponsors (53%) now allow specialist visits without a referral, although the majority (60%) requires higher cost-sharing for a specialist visit.
Despite these cost-sharing provisions, HMOs are no longer offered as a way to save money — they can’t compete in that arena with the low-cost consumer-directed health plan. Rather, they are more likely to be offered as the “rich” medical plan option. But even that role is threatened by the excise tax on high-cost plans.
