Managing Specialty Pharmacy Costs: What to Look for in the Data

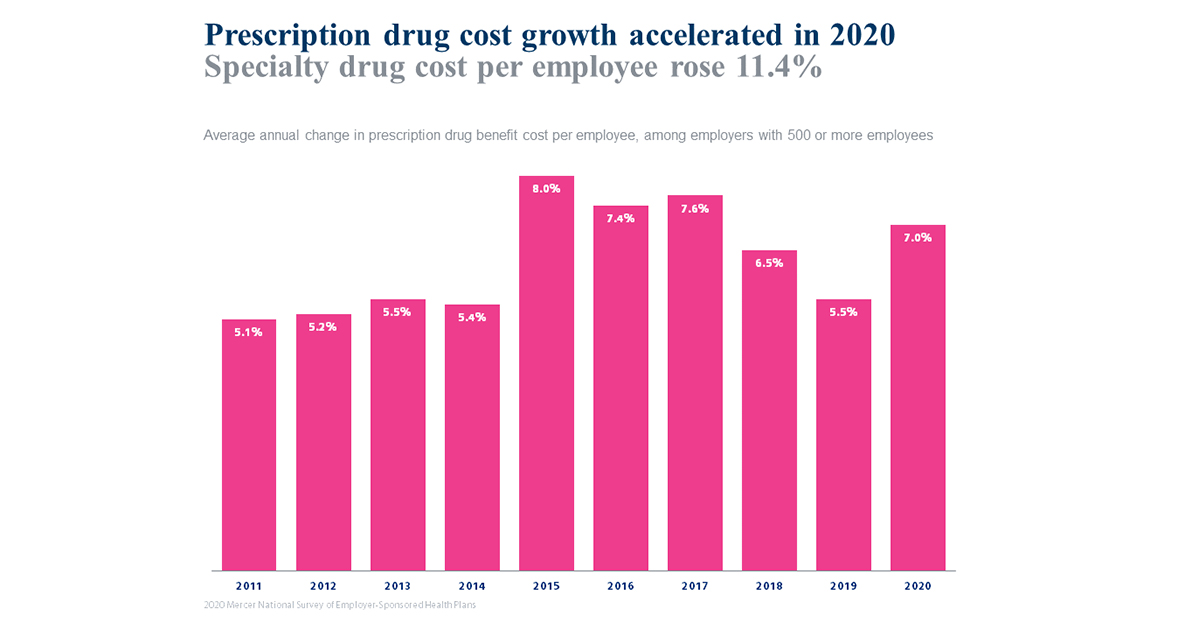
Prescription drug benefit cost growth continues to outpace other medical plan costs. While the average total health benefit cost per employee has been rising by about 3-4% annually in recent years (dipping lower in 2020 due to disruption in utilization), Mercer’s National Survey of Employer-Sponsored Health Plans found that large employers experienced prescription drug cost growth averaging 7% in 2020. Of note, those that track specialty drug cost separately reported an average increase of 11.4%, indicating that increased spending on these high-cost drugs is driving overall drug cost growth.
Specialty biotech drugs offer extraordinary breakthrough treatments for severe medical conditions such as HIV, multiple sclerosis, cancer and therapies for rare genetic conditions. However, they come with a very high price tag; a course of treatment can cost $100,000 or more. Even though these medications treat only 2% or less of the population, they account for 51% of drug benefit costs.
Delving into plan data can help employers manage this significant and growing cost. Here are six things to look for in your data to identify future opportunities to improve plan performance.
1. Drug spend. Analyze drug spend across both the medical and pharmacy benefits and project how those costs may escalate over time. This may influence plan design decisions: Employers are increasingly choosing to exclude coverage under the medical plan for some drugs to steer members to a specialty pharmacy (42% of large employers in 2020, up from 36% in 2019).
2. Rebates. Re-evaluate the financial value of specialty pharmacy rebates under the medical plan and negotiate contract language specifically focused on specialty medication. Rebate values are typically pretty low, but have the potential to increase as there are more carriers preferring drugs under the medical benefit. As competition grows for preferred drug placement under the medical benefit, rebate potential for those claims should increase.
3. Site of care. Know where plan members are receiving infusions – in a hospital, physician's office, or at home – and actively work with your PBM/carrier to drive distribution to the most efficient channels. EBRI estimates that the elimination of site-of-care price differentials for specialty medications could save employers and plan members between 4% and 36% depending on the medication.
4. Out-of-pocket costs. Examine PBM programs associated with their specialty pharmacies that maximize the amount of support the drug manufacturers may be willing to contribute to members’ out of pocket cost, potentially lowering employees’ cost to zero.
5. Integrated care management. Assess the care management integration between the PBM, specialty pharmacy, and medical case management. Look for repeated emergency room use or hospital admissions that may indicate opportunities to minimize drug side effects or other disease management interventions. A clinical pharmacy review can determine if appropriate guidelines are being followed.
6. Catastrophic claims risk. Look at your population demographics, diagnoses and claims history to gauge the risk of catastrophic cases that might require use of cutting-edge and extremely expensive medications or gene therapies. Then you can assess ways to mitigate the risk via authorization programs, stop loss coverage and captives, to name a few approaches.
In short, knowledge is power. If you’re not using your data to the fullest extent to help manage specialty drug costs, now is the time to start. With new gene therapies just starting to come to market and many more in the pipeline, it’s important to get these processes in place so you’ll be ready when they are.
