This Open Enrollment, Think of Employees as Shoppers

The theme of our annual open enrollment webinar this year (in addition to required disclosures, of course!) was how to engage employees in the benefits shopping experience during open enrollment and throughout the year. In case you missed it, here are three take-aways:
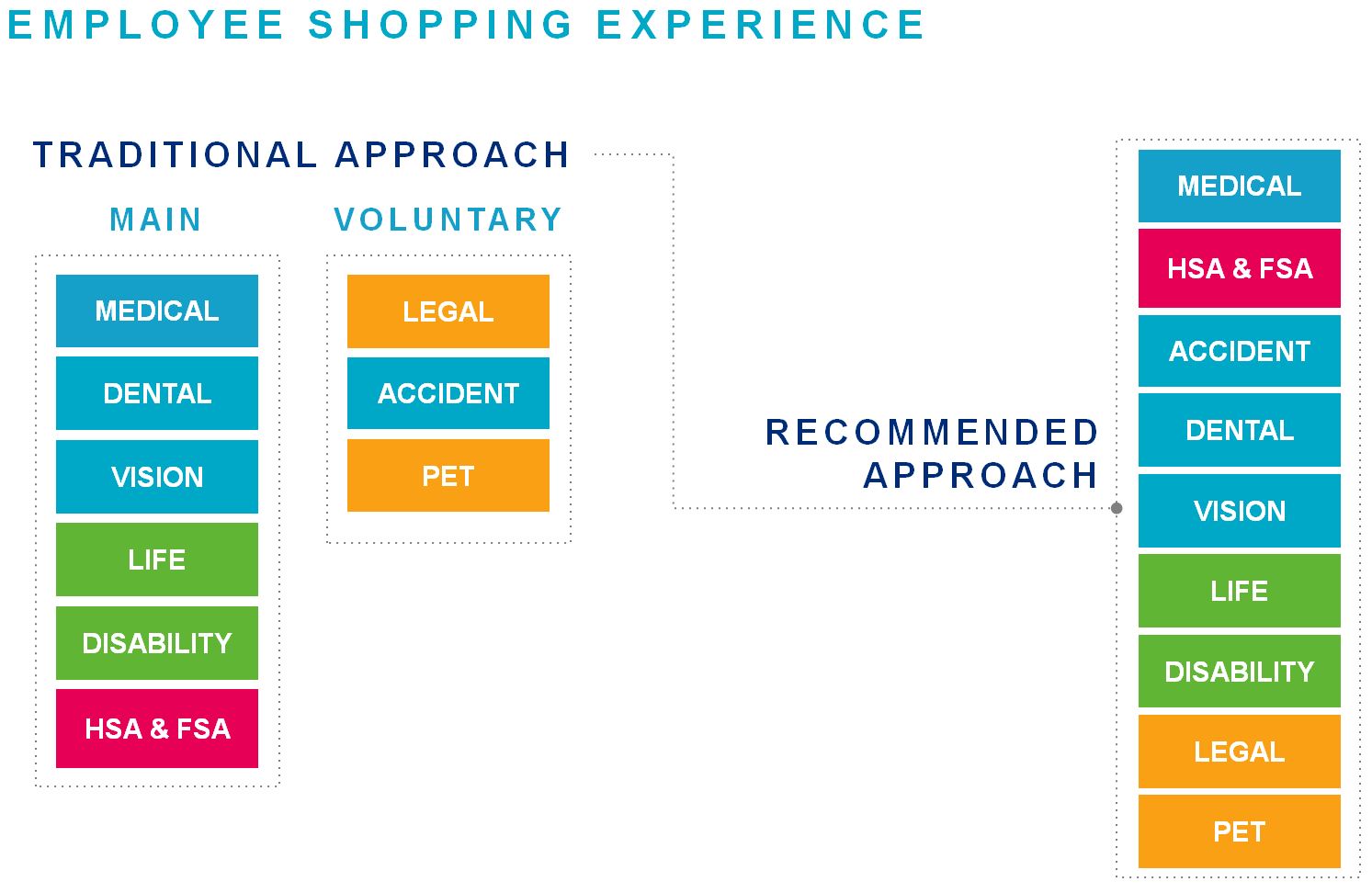
Shake up the order. Retailers know it matters where merchandise appears in a store, catalogue, or website. We’ve learned through our experience of assisting employers that the order in which benefits are offered to employees affects participation. Typically, medical, dental, and vision benefits appear first in all enrollment materials. Health savings accounts or flexible spending accounts are offered at the end of their enrollment experience and voluntary benefits may be offered through a separate site. We’ve found that an integrated enrollment site improves the employee’s experience and increases awareness and value of voluntary benefits offerings. Consider moving HSAs and FSAs after medical and follow with accident and other supplemental health policies that can be used by employees to complement their medical plan.
Encourage informed decision-making. Employees value choice in their benefits offerings. In our experience, employers who offer meaningful choice will see a material number of employees select each plan option. Of course, true success in a choice environment means each employee is making optimal selections for themselves and their families. The best way to achieve that goal is to make decision support tools available -- and take steps to ensure that employees actually use them. Make them simple and quick to use, personalize the support where possible, and embed the support to appear at the appropriate time on your enrollment platform.
Keep them coming back for more. Engaging employees in the benefits shopping experience shouldn’t end at open enrollment. Selecting a health plan and a portfolio of benefits is important, but so is selecting healthcare providers. Transparency tools are information resources that detail individual provider cost and quality ratings. With 29% of covered employees enrolled in a high-deductible health plan and 72% of large employers expected to offer a consumer directed health plan in 2019, transparency tools are becoming more important than ever. Don’t be put off by low utilization – it doesn’t appear to be driven by opposition to the idea of price shopping for healthcare services but rather the difficulty in obtaining price information. With 800 – 1,600+ medical services and 4,000+ prescription medications that are shoppable, there are plenty of opportunities for employees to become better consumers of health care services -- you just need to get them engaged. In 2018, 82% of employers will offer transparency tools, but (according to a 2017 Consumer Health Mindset survey) fewer than 50% of consumers know where to get cost and quality information. If you offer a transparency tool, make sure employees know about it! Make it easy to access, make the information understandable and give employees a reason to use it.